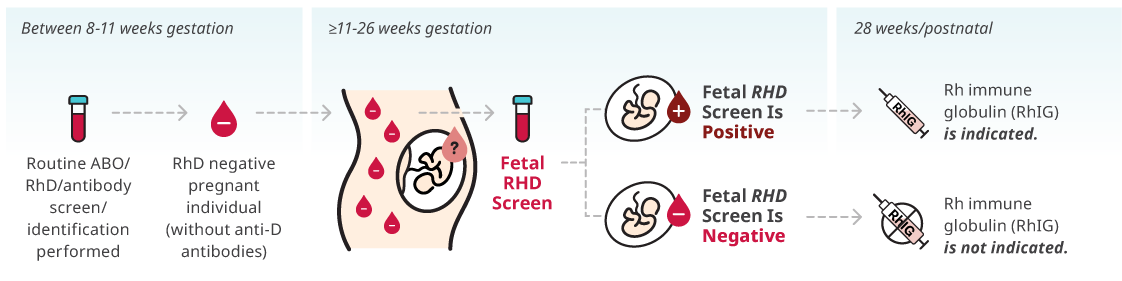
RhD can cause problems in pregnancy if you are RhD negative and your baby is RhD positive. This is called RhD incompatibility.
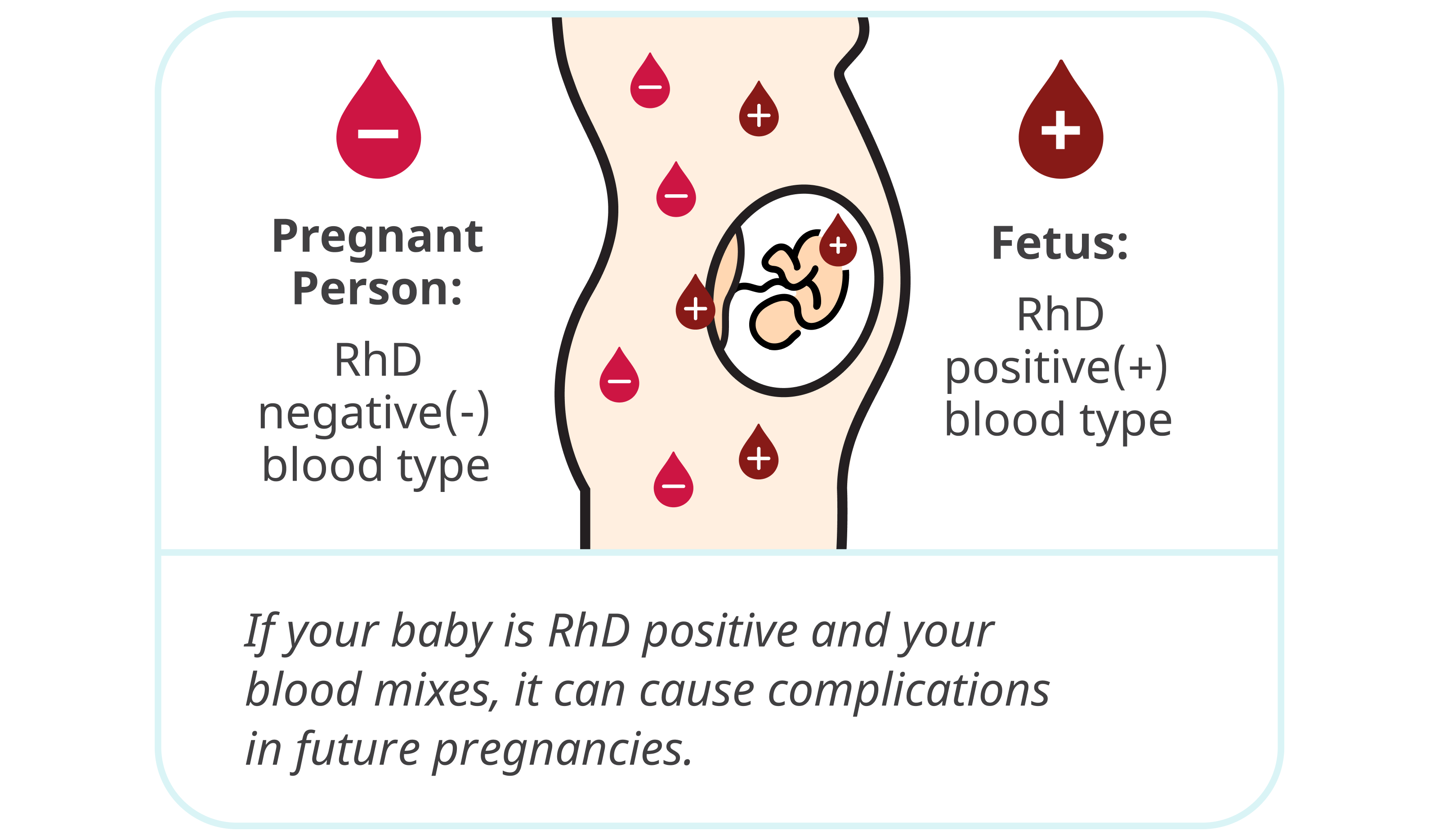
What happens if there is an RhD incompatibility?
If your RhD negative blood is exposed to your baby’s RhD positive blood, your immune system can make antibodies (called anti-D) against your baby's mismatched blood. This is called RhD alloimmunization (or sensitization) and can happen if your baby’s blood mixes with yours during pregnancy or at delivery.
In rare cases, the baby may need a blood transfusion, before or after birth. The symptoms of HDFN can range from mild to severe. Not all babies will have symptoms. Most babies recover within a few weeks and have no lasting problems. Careful monitoring and treatment during pregnancy and after birth can prevent most serious problems.